As seasons change people are affected with different types of skin infections irrespective of their age or skin type. Whether it is the moist monsoon fungal infections, the dry and humid summer rash or the cool winter eczema such changes in the weather create the perfect environment that is required by the organisms like bacteria, fungi or even worms to thrive in it.
Once such infections are onboarded people tend to try out different methods and solutions to get rid of them. These solutions range right from the basic topical ointments and medications to natural treatments or even remedies that our elders have used. But which of these remedies is actually helpful in treating these infections and also does one type of remedy have an edge over the other?
Seasonal Skin Infections
Seasonal skin infections are very common due to changing weather conditions that affect the skin.
Summer brings excess sweat and humidity, leading to fungal infections like ringworm and athlete’s foot, as well as acne and sunburns.
- Summer Fungal Infections: Heat and humidity cause excessive sweating, creating a breeding ground for fungi like those causing ringworm and athlete’s foot.
- Acne: Clogged pores from sweat and oil can lead to acne breakouts.
- Sunburn: Prolonged sun exposure can cause sunburn, characterized by redness, peeling, and pain.
- Heat Rash: Blocked sweat ducts can lead to heat rash (prickly heat), causing small, itchy bumps.
Monsoon season with high humidity can exacerbate fungal infections and eczema,
while the dry air of winter can cause dryness, itchiness, and cracking.
- Monsoon Fungal Infections: High humidity promotes fungal growth, leading to conditions like ringworm.
- Eczema: Increased moisture can aggravate eczema, causing flare-ups of redness, itching, and dryness.
- Bacterial Infections: Dampness can create an environment for bacterial infections.
Winter Dryness and Itchiness: Cold, dry air removes moisture from the skin, leading to dryness, itching, and cracking. Also, Winter weather can worsen eczema symptoms.
Spring & Autumn: Allergies: Transition periods trigger allergies, causing rashes and skin irritation.
Common Types of Seasonal Skin Infections
1. Fungal Infections
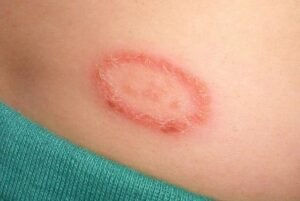
- Ringworm (Tinea): Circular red itchy patches
- Athlete’s foot: Cracks or scaling between toes
- Candidiasis: Affects moist areas like underarms or groin
Trigger: Monsoon and summer due to excess sweating and moisture
2. Bacterial Infections
- Folliculitis: Infection of hair follicles
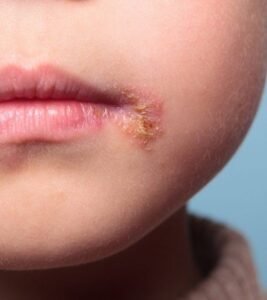
- Impetigo: Honey-colored crusts, especially in children
- Cellulitis: Red, swollen painful skin, often on the legs
Trigger: Humid weather, skin injuries, poor hygiene
3. Viral Infections
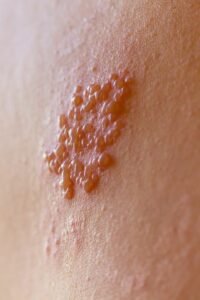
- Herpes simplex: Cold sores or genital lesions
- Molluscum contagiosum: Small flesh-colored bumps
- Chickenpox/Shingles: Painful itchy blisters
Trigger: Weak immune system, seasonal drop in immunity
4. Allergic or Inflammatory Skin Conditions
- Eczema and Dermatitis
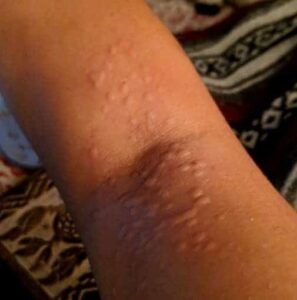
- Hives (Urticaria)
- Photosensitivity rashes
Trigger: Dry winter air, seasonal pollen, or UV exposure
Why Do They Occur Seasonally?
Changing seasons affect:
- Skin barrier function: Dry winter air or wet monsoon conditions compromise the skin’s defenses.
- Sweat and oil production: In summer, increased sweat creates a breeding ground for fungi and bacteria.
- Allergen exposure: Pollen, dust, and mold increase in specific seasons.
- Reduced immunity: Cold weather lowers immune response, making it easier for viruses to cause skin issues.
Medical Remedies for Seasonal Skin Infections
1. Antifungal Creams and Tablets
- Clotrimazole, Miconazole, Terbinafine: For ringworm, athlete’s foot, and candidiasis.
- Oral antifungals for persistent or widespread infections.
2. Antibacterial Ointments
- Mupirocin, Fusidic acid, or Neomycin: For impetigo, folliculitis, and infected cuts.
3. Antiviral Drugs
- Acyclovir, Valacyclovir: Effective for herpes simplex and shingles.
4. Antihistamines and Steroids
- For hives, eczema, or inflammatory skin conditions due to seasonal allergens.
If parasitic infections are suspected, doctors may recommend antiparasitic medications like Iveocop 6, particularly in regions where skin exposure to contaminated water or soil is common during monsoon.
Home Remedies and Natural Treatments
While medication is essential in many cases, natural remedies can complement your treatment:
1. Coconut Oil
- Antifungal and soothing
- Great for fungal infections and dry skin
2. Tea Tree Oil
- Antibacterial and antifungal
- Apply diluted (never directly) to rashes or fungal spots
3. Neem (Indian Lilac)
- Powerful antifungal and antibacterial
- Use in baths or apply neem paste to affected areas
4. Cold Compresses
- Relieve itching and inflammation in hives or eczema
5. Aloe Vera Gel
- Soothes irritated skin, boosts healing
Note: Natural remedies should be used with caution and not as a substitute for proper medical care.
Preventive Tips to Avoid Seasonal Skin Infections
Maintain Hygiene
- Bathe daily with mild antiseptic soap
- Keep skin folds dry (underarms, groin)
Wear Breathable Clothes
- Especially in summer and monsoon
- Avoid tight synthetic garments
Moisturize in Winter
- Prevents dry skin, cracking, and eczema flare-ups
Avoid Sharing Personal Items
- Towels, razors, socks, etc. can spread infections
Boost Immunity
- Eat vitamin-rich foods, stay hydrated, get enough sleep
Use Protective Creams
- Barrier creams for eczema
- Sunscreen for UV-triggered rashes
If you’ve had recurrent parasitic skin issues during rainy seasons or travel, a preventive course of Iveocop 6 may be suggested under medical supervision.
When to See a Doctor
- Persistent or spreading rash
- Painful blisters or open sores
- Pus, swelling, or fever
- No improvement with home care in 3–5 days
Key Takeaways
- Seasonal skin infections are common and usually caused by fungi, bacteria, or viruses during specific weather conditions.
- Types include ringworm, impetigo, herpes, folliculitis, and eczema.
- Treatment includes antifungal, antibacterial, or antiviral medications based on the underlying cause.
- Irritation, itching, and skin damage can often be prevented by following basic hygiene and seasonal skin care routines.
- Natural remedies like neem, tea tree oil, and aloe vera can support healing but should not replace medical treatments.
- Seek medical attention if the condition worsens or does not respond to home remedies.
FAQs
1. How do you get rid of skin infections naturally?
Natural remedies:
- Aloe vera – Perhaps you’ve used aloe vera in the past for a sunburn, yet the gel-like substance from the leaves of this subtropical plant may be used for other skin problems, too.
- Honey
- Lavender oil
- Marigold
- Turmeric paste
- Tea tree oil
- Topical vitamin E
2. How to treat seasonal skin allergies?
Antihistamines and moisturizing ointments can help ease irritation and dryness.
Recently, new medications have been approved, including:
- An ointment for mild to moderate atopic dermatitis
- A biologic for moderate to severe atopic dermatitis
You can discuss these options with your allergist.
3. What is the fastest way to cure a skin infection?
With antibiotic treatment, signs and symptoms of skin infections begin to improve after approximately 2 to 3 days.
If your skin infection does not improve or gets worse (especially if you develop a fever or the infection spreads), notify your doctor right away.
4. What is the most powerful natural antifungal?
Many natural remedies boast antifungal properties, but tea tree oil often takes the crown as the most potent.
Garlic is another strong contender, thanks to its allicin content.
5. How can I speed up the healing of a skin infection?
Your body needs good food to fuel the healing process.
Include foods rich in vitamin C in your diet — the body needs it to make collagen.
Fresh fruits and vegetables eaten daily will also supply your body with other nutrients essential to wound healing such as:
- Vitamin A
- Copper
- Zinc